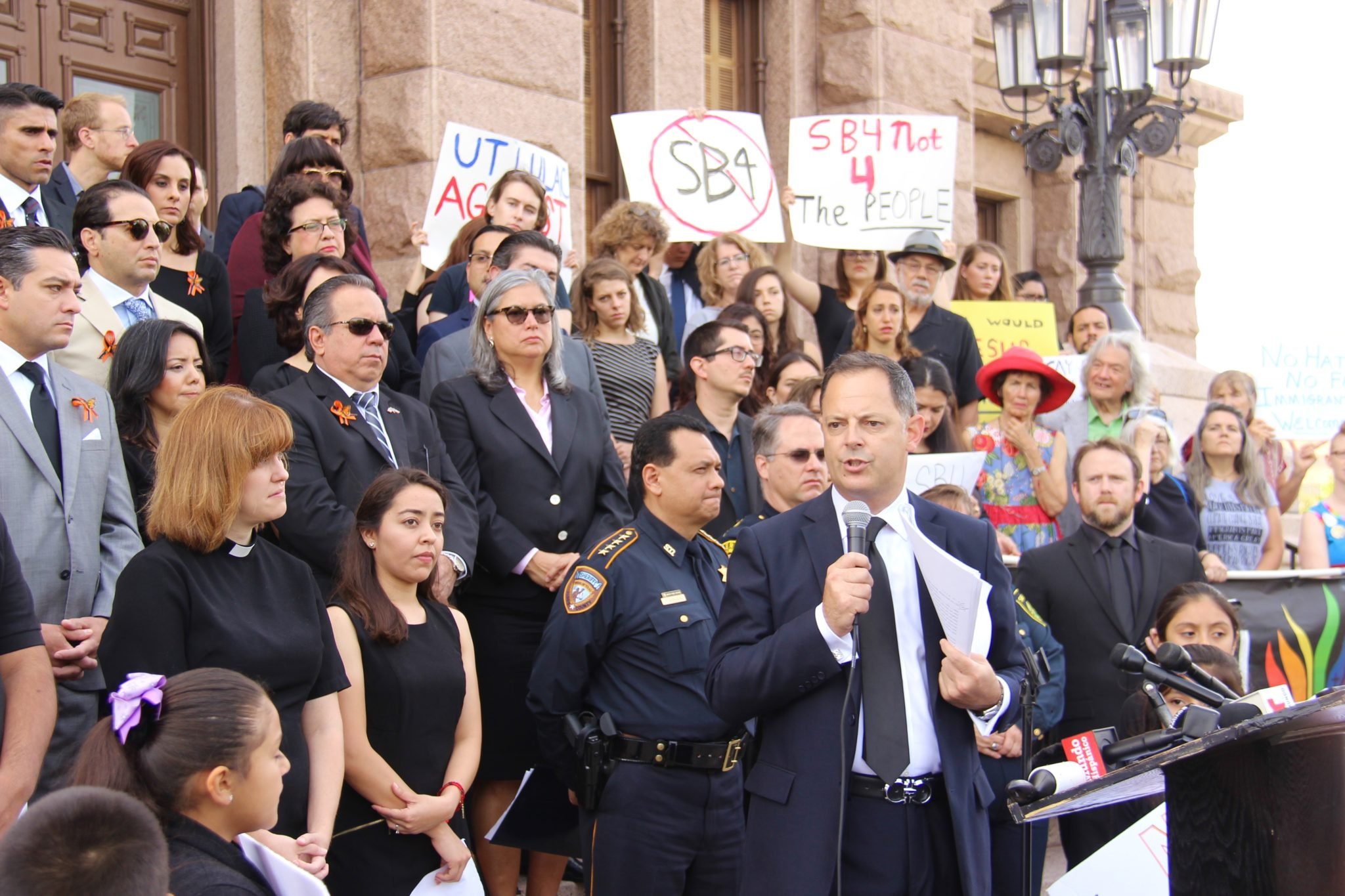This story is part of a continuing series on the dismantling of women’s healthcare in Texas.
The fetus Michelle was carrying was dead. At her 14-week checkup, the doctor had detected only low cardiac activity. Now, two weeks later, the physician confirmed it: The fetus likely had been dead for most or all of the intervening time. The 35-year-old Missouri woman, who asked that her real name not be used, vividly remembers what her doctor said next.
“If there’s one thing I want you to go away understanding, it’s that you are in mortal danger,” she told Michelle.
Because she had been carrying a dead fetus for so long, Michelle was at risk of developing sepsis or an infection. “Either could be fatal. I needed to make a choice quickly,” she recalled. Her two options were to receive what’s called a D&E—a dilation and evacuation, the procedure also used for second-trimester abortions—or to be induced and go through labor.
“I said immediately, ‘Well that’s easy, of course I want the D&E. Why would I want to go through labor for a dead fetus?’” Michelle said. “That’s awful.”
But Michelle’s OB-GYN worked at a hospital that didn’t provide D&Es. “It’s perceived as an abortion by the community,” a nurse explained.
The closest doctor who could perform the procedure was an hour and a half away in Kansas, and he didn’t feel comfortable treating her right before he left for a vacation. When she called around, and other doctors said they couldn’t do the D&E either, she asked why. They told her no one in the rural area was properly trained in abortion techniques, including the technique she needed for her miscarriage.
Michelle had no choice but to be induced. She went through 21 hours of labor that traumatized both her and her husband.
That was in 2018. “When Roe v. Wade got overturned, immediately I started thinking about my miscarriage. I was very upset,” Michelle said. “I thought, ‘Oh my god, how many women aren’t going to be able to get a D&E when they need one?’”
Texans are now grappling with the same problem. The statewide abortion ban triggered by the Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization in June 2022 has made it harder for women to get the care they need. But it has also made it harder for fledgling OB-GYNs to learn necessary skills during their residencies, the four years of specialized training after medical school.
Why would a lack of abortion skills matter in a state that has outlawed almost all abortions? Because the surgical techniques used for elective abortions are used in other aspects of OB-GYN care, particularly in treating miscarriages. The situation threatens to cut off Texas’ supply of well-trained OB-GYNs equipped to provide both basic and critical care to all Texas women. Experts worry new doctors will leave the state for a higher caliber of training—and that they won’t come back.
All OB-GYN residency programs must offer clinical abortion training to remain accredited by the Accreditation Council for Graduate Medical Education (ACGME), the governing body of all U.S. residencies—even if abortion is illegal in the state. Students can decline the training on moral or religious grounds. The ACGME reaffirmed the requirement after the Dobbs decision.
That means the 23 Texas OB-GYN residency programs must find the means and the money to provide their students with abortion training, even though the hospitals where the programs operate cannot provide elective abortions—or almost any abortion procedure—to patients. “It’s quite an uphill battle for us to get them to the place they need for their training,” said Dr. George Barnett, program director of the OB-GYN residency at Texas Tech University Health Sciences Center at Amarillo. If programs don’t find a solution, they are at risk of losing their accreditation and shutting down.
One potential answer is sending medical residents out of state for their abortion training. But the travel solution ushers in a barrage of its own problems. For instance, the duration of such training might not provide the skills that OB-GYNs need to help patients in serious, sometimes life-threatening situations.
“I think it endangers our healthcare system,” said Dr. Ghazaleh Moayedi, an OB-GYN in Dallas. “In general, we’re not going to be able to recruit and continue to recruit talented physicians. As the Legislature continues to encroach on the practice of medicine, it is going to discourage people from practicing medicine here.”
Navya Kumar, a fourth-year medical student in Houston, is worried about her own future in the field. She’s currently interviewing with OB-GYN programs inside and outside of Texas. “I’m feeling pretty bad, I would say, just generally,” she said. “It’s going to be really, really hard to be an OB-GYN moving forward. It just… sucks.”
Programs across 14 states with abortion bans are grappling with the training problem, but Texas institutions have been dealing with it for quite some time. “What we are seeing now isn’t new,” said Dr. Anitra Beasley, a professor in the OB-GYN residency program at Baylor College of Medicine. “The restrictions regarding abortion training have been long-standing.” But the stricter ban and closure of all abortion clinics made the problem even worse.
Over the last several decades, Texas legislators have steadily passed laws making it more difficult for people to access abortions, for physicians to provide them, and for students to train for them.
House Bill 2, passed in 2013, required doctors administering abortions to have admitting privileges at a hospital within 30 miles of the abortion clinic and required the clinics themselves to meet the standards of mini-hospitals. Parts of the bill were eventually struck down in 2016, but the damage was already done: 27 of the state’s 42 abortion clinics closed. Six Texas OB-GYN residency programs were left without an abortion clinic within city limits.
Then in September 2021, Senate Bill 8 restricted abortions to the period before fetal cardiac activity can be detected (around five or six weeks gestational age), effectively banning most elective abortions. Surgical abortions are legal if the mother’s life is at risk or if cardiac activity can no longer be detected. This all but eliminated the ability for medical residents to learn how to perform abortions during routine procedures.
“Medical school education around abortion and contraception has been woefully inadequate in our state for quite a while,” Moayedi said. Medical schools (as opposed to OB-GYN residency programs) are not required to provide abortion training, but some students seek out extracurricular instruction. In a popular workshop run by Medical Students for Choice, OB-GYN residents use papayas to demonstrate how to use abortion tools.
“It’s kind of similar to a uterus,” said medical student Kumar, who has attended a workshop. “The shape is not it, but the seeds are in the right place, so you could do it.”
Dr. Esha Singhal, a first-year OB-GYN resident at Baylor Scott & White All Saints Medical Center in Fort Worth, said her program is doing whatever it can to provide the training residents want. “The hope is, no matter your political beliefs, we come out of residency able to do what we need to do,” she said. The organizers of her program have been discussing sending residents to other institutions for abortion training.
Even before the more restrictive abortion laws, only OB-GYN residents in cities with abortion providers, like Houston and Austin, could commute daily to a clinic within city limits without needing to relocate, said Kristin Simonson, director of programs and operations at the Ryan Residency Training Program, an organization that helps OB-GYN programs integrate abortion training into their curriculum.
But many programs did not have abortion clinics nearby. Texas Tech Health Sciences Center at Amarillo partnered with the Ryan Program to send residents to Dallas, 365 miles away, to train for two weeks at a Planned Parenthood clinic, said Dr. Barnett, director of the OB-GYN residency at the Amarillo school.
Now the travel distance is on the scale of plane rides rather than car rides. Residents with children or other family members to care for are put in a “difficult place if they want the training but can’t afford to be away,” Simonson said.
Traveling for training is also expensive: Costs include housing, transportation, malpractice insurance, and a medical license to practice in another state. Program budgets sometimes only cover work students do at their home institution, Baylor’s Dr. Beasley said, so the cost of out-of-state training can fall on the student.
When Moayedi was a medical student in Fort Worth, she traveled to San Francisco for a one-month family planning rotation. There wasn’t a way to receive training locally through her school. “It really became my own responsibility to find [abortion] training,” she said. The rotation was elective, so she had to pay for it herself. She ended up taking out additional student loans. “It was burdensome on time. And it was a lot of money I had to borrow to be able to do that. But it was worth it for me. But that’s a huge barrier for people,” she said. During her residency in El Paso, she didn’t receive any abortion training because the clinic her school partnered with kept opening and closing in response to changes in legislation.
After the Dobbs decision, abortion clinics in many states closed down. Remaining clinics are overwhelmed with students who need to train there. “What is existing right now can’t absorb the training needs of the rest of the country,” Moayedi said. In states where abortion is protected, “We need new places doing abortions, so we can have new places training [for] abortion care.”
Other physicians agree. “I think [traveling] is a good temporary measure, but I just worry that it’s not sustainable,” said Dr. Cece Cheng, a fellow in maternal-fetal medicine in Texas. Following the passage of Senate Bill 8, Cheng’s institution, which she asked not to be named, set up relationships with institutions in other states so residents could complete their abortion training.
“There’s only a certain number of patients available and everyone needs to be trained. And so of course, [the priority at] other institutions is going to be training their [own] residents and fellows,” Cheng said. Some of her institution’s travel relationships ended once the Dobbs decision increased the demand for out-of-state training.
Another problem with travel is that training becomes confined to a single two-to-four-week period. “That probably isn’t all the time that you would need in order to gain the skill set,” Beasley said. “Even if you have the ability to go somewhere else and do this training, there’s still not the same guarantee that you’ll be able to get the volume of procedures that you need.”
Residents are required to perform at least 20 surgical abortions to satisfy the ACGME’s requirements. Beasley and other physicians worry that simply meeting this requirement isn’t enough to develop adequate skills. The main techniques used to perform a surgical abortion are called dilation and curettage (D&C) and dilation and evacuation (D&E). They both entail dilating the cervix and then emptying the uterus through different methods. Both procedures are also used for managing miscarriages; about half of miscarriages are treated with D&Cs.
In states where abortion is legal, residents first learn those surgical skills in a concentrated rotation and continue to practice them for the rest of their four-year residency. Texas OB-GYNs-in-training would only be able to practice during their two-to-four-week rotation.
Singhal, the first-year resident in Fort Worth, isn’t worried about reaching the 20-procedure minimum. “D&C is not one of the most complex procedures,” she said, and her hospital performs enough medically required abortions that “I will know what I need to know at the end of my residency.”
Some physicians aren’t so sure. They worry that Texas OB-GYN residents may not get the level of exposure and practice from routine abortions that would equip them to handle more severe complications, like when a patient needs an emergency D&E.
“Let’s say they have a severe infection, or they are hemorrhaging. Minutes matter,” said Beverly Gray, program director of the OB-GYN residency at Duke University School of Medicine. “Not only are those patients at risk, but the residents caring for those patients are not able to get the experience managing those cases, which are unfortunately common cases in our field.”
When young doctors lose the opportunity to develop these critical skills, it could translate into a loss of institutional knowledge throughout the field as older doctors retire. Cheng described it as a domino effect: Doctors who stay in Texas for their training won’t be able to train the next generation on how to perform abortions.
Gray said the problem persists even if abortion bans are eventually overturned. “In that period of time, there’s this collective loss of skill that I think could completely erode the ability to have experts that are training the next generation.”
And if Texas medical students have to go out of state for their OB-GYN residencies, there’s a good chance they will never come back. About 52 percent of OB-GYN residents practice medicine in the same state where they completed their residency. “I worry that this is going to make Texas even more of a healthcare desert,” Cheng said.
Texas OB-GYN program residencies might start to see a drop in applicants, but Beasley, at Baylor, said it is too soon to tell. Program officials interviewed applicants earlier this year for residencies to start in June or July. Applicants were to be matched with institutions in March. Both faculty and applicants said access to abortion training has been heavily discussed in interviews.
“We had a lot of questions about what’s happening and how we manage patients and what our perspective is,” said Barnett, the program director at Texas Tech University Health Sciences Center at Amarillo.
Kumar, the fourth-year medical student in Houston, is interviewing with OB-GYN programs across the country. She said state abortion laws did not influence where she applied but will play a role in how she ranks her choices after finishing interviews. She wants to practice in Texas or another state in the South. She is passionate about providing patients with OB-GYN care that is as supportive as she can make it within the limits of the law.
“I will stay here and fight for that as long as it takes,” she said. “I’m not tired enough, I haven’t been beat down enough to leave. Maybe for my residency, but not for my whole life.”