The Emergency
Houston's emergency care system is in critical condition. Can it be saved?
Houston City Bus # 1 begins its loop in a gritty North Houston neighborhood of tire shops, wrecking yards, and all-but-abandoned hair salons. The marquee on the front of the bus simply says “Hospital.” It winds through streets grown up in magnolias and banana trees, past two-room houses, some brightly painted, some nailed shut, then heads downtown to cruise by some of Houston’s fanciest hotels. The bus reaches its far terminus in the small city of hospitals, pharmacies, administrative buildings, and parking garages that is the Texas Medical Center.
On the Friday before Labor Day weekend, at around six o’clock in the afternoon, the front of the bus is overflowing with members of one anxious family. The Ramirezes shift seats continuously to take turns fussing over 20-month-old Rebecca, who does or does not have a fever of 101 or higher, depending on whom you ask. She looks flushed and heavy-lidded, but then, she is swaddled head to toe in a Spiderman blanket and the temperature outside is in the 90s. To be on the safe side, however, her mother, grandmother, uncle, and two aunts, are taking her to the emergency room at Ben Taub General Hospital to see a doctor.
The grandmother, who speaks no English, fusses ceaselessly over the baby, fluffing her small pigtails, or pulling the blanket tighter around her feet. Rebecca’s mother, Irene, is calmer.
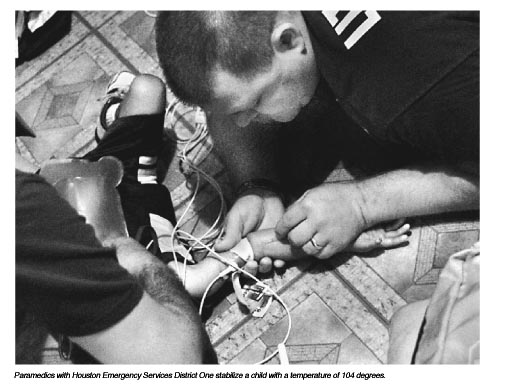
“You can feel she’s really hot,” she says. “I’m worried, because it’s Friday and I don’t want her to be sick all weekend. But my mother is the most worried. In Mexico, you know, she knew women who had babies die. This is her only grandbaby. So she worries.”
Rebecca has made the trip to Ben Taub twice before, once for a fever and ear infection, once for a crying fit that wouldn’t stop. Rebecca is covered by the Children’s Health Insurance Program, and has a regular physician she sees for check-ups a few times a year. But the trip to the pediatrician’s office from the Ramirez home requires three bus changes, and the office closes at 5:30 p.m. Since everyone in the family works, it’s hard to take Rebecca to see him. “I know his name, but I talk more to his answering machine,” Irene says.

The bus pulls into the circle drive at Ben Taub, and the Ramirezes climb out. In Ben Taub’s emergency waiting room, they sign a list and sit down—to wait. The room is beginning to fill with the usual Friday afternoon rush, compounded by the long weekend ahead. There are many families with children, several pregnant women, and scores of others whose slumps and twisted faces testify to their pain. One old woman passes her hand across her face repeatedly, without pause. A man at the nurses’ desk pleads to have his prescription filled.
The nurse’s face glistens from exhaustion. “You can sign the list and sit down,” she tells him. “But this is Friday night. This is a trauma night. The wait for you will be many, many, many hours.”
In fact, for “non-emergent” cases at Ben Taub, the average wait to see a doctor is around 12 hours. For those sick or injured enough to warrant a bed in the surgical or medical bays, it is closer to six hours. The most severe cases are seen as soon as possible—a sliding measure that depends on how many beds are open, how many doctors and nurses are on call, how fast the beds are cleaned once they are cleared, and how many even worse cases are already waiting. Trauma experts talk about the “golden hour”—the 60-minute window during which, if treated, a trauma patient has the best chances of survival and recovery. After that hour, those chances go down. At Ben Taub, hospital policy dictates a physician see the most serious cases within 30 minutes. But like most emergency rooms in Harris County—and a growing number across the state—Ben Taub is sometimes precariously close to letting the golden hour pass.
“We are on the verge of not being able to provide safe care because of the sheer volume of people coming in,” says George Masi, Ben Taub’s assistant director of emergency services. “Because emergency rooms have become in many ways the sole source of care for so many people, they’re just overwhelmed. Every day is a crisis, all day long.”
Toward midnight, a small man with an Astros cap pulled low wheels his wife into Ben Taub’s emergency waiting room on a gurney borrowed from the hospital. She is moaning under her white sheet, a continuous, high-pitched sound like a baby crying. Her husband explains to a nurse at the triage station that she has an abscess on her leg “this size”—he shows his fist—and that her painkillers aren’t working. She woke herself up with her own screaming nearly two hours ago and hasn’t stopped since. Their 10-year-old daughter stands at her mother’s head, nodding solemnly. The nurse tells the family to sign the list and sit down until their number is called. But there’s nowhere to put the gurney. The father and daughter won’t leave the woman by herself, and so the three stay by the nurses’ station, waiting for something to happen. Ten minutes later a nurse’s aide moves the woman’s gurney around a corner, but you can still hear her. The daughter paces back and forth to the nurses’ station; every few minutes she asks again when her mother will be seen. The nurses try to explain—there are lots of sick people, people who need help right away. Mom has to wait.

Fifty minutes later the woman is still waiting, and still moaning. Finally, the family gives up. Her husband curses, wheels the gurney around and heads back down the hall to the front entrance, and out into the parking lot. The girl trails them, then runs to get the door of the station wagon, as the man lifts his wife up tenderly in her sheet. They settle her into a nest of blankets in the back seat, then slam the doors and drive away. Inside, the Ramirezes are still waiting.he Emergency Center at Ben Taub sees around 300 patients a day, at a hospital with a total of 600 beds. “We are overcrowded by any possible measure,” George Masi says. It is not the only emergency department in Harris County that can make that claim. Virtually all—big and small, private and non-profit—experience periods of over-crowding so intense that they route ambulances away to other hospitals, a process called “diversion” or sometimes “drive-by.” A 2002 study commissioned by Houston non-profit Save Our ERs found the mortality rate of trauma cases doubles when both of the region’s Level I trauma centers—the centers that take the most severe trauma cases—are diverting ambulances. In recent months, they have been on drive-by nearly 30 percent of the time.
While the entire hospital system in Harris County is strained, Ben Taub is bearing a heavier burden than most. As the flagship facility of the Harris County Hospital District, the hospital is charged with caring for the county’s poorest residents. Those patients—the ones with Medicaid, CHIP, or with no insurance at all—account for the majority of emergency room visits. Not all of them need emergency medicine; many are merely sick with the sore throats and earaches that any other doctor could treat. But they have no other doctor, and that, in its way, is also an emergency.
Masi estimates as many as 30 percent of the patients who come to the Ben Taub emergency center do not have genuine emergencies. That’s not to say that they don’t need to see a doctor—a tricky proposition if you’re poor in Houston. The waiting list at one of the city’s public community clinics may be anywhere from a few weeks to a few months long. Those who get an appointment may not be able to take time off during the workday. Private physicians and clinics are reluctant to take Medicaid patients because the state’s reimbursement rates are lower than market rates—and the uninsured might as well forget about private care. It’s not unknown for private physicians to refer an unwanted patient directly to the ER.

In contrast, emergency rooms are open 24 hours a day, and on weekends. By federal law, no ER, public or private, can turn anyone away, whether or not they can pay for treatment. The Medicaid co-payment for non-emergency services delivered at the emergency room is a bargain at $3. (The state can charge double that amount, if they prove you had an “alternative” avenue of care available, but that’s a lot of trouble to go to for an extra three bucks.) And for the uninsured and indigent, ERs routinely waive fees due to inability to pay.
Non-emergency patients are a burden on the ER. But the worst cases are those who avoid care until a minor condition becomes a full-blown emergency. Patients who wait for an emergency—for the high blood pressure to become a stroke, or the lacerated hand to become infected—have worse chances of recovery. And their treatment is more expensive.
“Because this is a hospital that treats the uninsured or underinsured, patients don’t access healthcare in other sectors like they would, so when they come to us, many times they are very sick,” Masi says. “The majority of our business is taking care of very sick people who are here as a result of lack of preventive medicine, or lack of intervention at an earlier stage of the disease.”
Most healthcare experts agree that lack of insurance is the single biggest factor crowding emergency rooms and that the problem is getting worse. “If insurance were extended to everyone in the population, this would disappear in six months. I’m sure of it,” says Save Our ERs founder Dr. Guy Clifton, who is chief of neurosurgery at Houston’s Memorial Hermann Hospital. Unfortunately, Houston has high numbers of those populations least likely to be adequately insured—the elderly, the working poor, immigrants, and children. And with the population of Texas projected to look more and more like Houston over the next few decades, the strain on the state’s emergency rooms is expected to grow.
“If you shut every other door except the door to the emergency room, guess where people are going to go in,” says Ron Cookston, executive director of Gateway to Care, a non-profit that collaborates with area hospitals to improve healthcare access for the poor and uninsured.
About 30 minutes north of Ben Taub on Highway 59 is Aldine Mail Route Road. Looping left, you pass the Nothing Over 99 Cents Store and A-Z Everything Under One Dollar, then a Church’s Fried Chicken and a strip mall whose only surviving enterprise is the Army-Navy Recruitment Center. A few blocks south of Aldine, in a rural-feeling neighborhood of trailer homes, big trees, and the odd chicken, is the Isom Road Station for Harris County Emergency Services District One. Two modest, vinyl-sided buildings at either end of a 40-foot concrete slab, the station is easy to miss, but serves one of the largest and poorest EMS districts in Harris County—an area that spans quiet blue-collar neighborhoods, gang turf, government housing projects, and urban colonias.
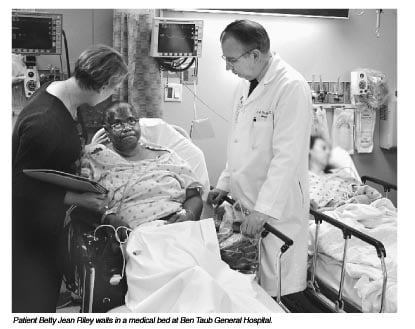
“Out here we are their medical services,” says paramedic-in-charge Laura Powell. “This is not a healthy area. We have a lot of older people, a lot of low socio-economic people, a lot of very sick people. We also have people who just need a ride to the hospital to get their prescriptions filled, and there’s no one else to take them.”
Ambulance crews out here answer a high volume of trauma calls—calls for rapes, beatings, stabbing, shootings, car-jacking, psychotic episodes, and drug overdoses. In recent years, with its open fields and wooded areas, the district has also been something of a body dump. But with a large population of the elderly and uninsured, the bulk of calls are for cases where neglect and non-compliance—not taking medications, or following dietary and lifestyle guidelines—have exacerbated existing illnesses to the breaking point.
“You do see sick people who probably shouldn’t be sick,” Powell says. “You end up doing a lot of patient education. You see things while you’re at a site, and you say “Oh, by the way”—though sometimes you’re thinking “Oh, my God!”
Late on Sunday afternoon, the crew of Medic 92 from the Isom Road station takes a 911 call phoned in from a McDonald’s by the freeway. When they arrive, a sandy-haired woman with a collapsing ponytail is slumped alone over a plastic-topped table, her arms folded tight across her stomach. Derrick Samuel and Jeremy Manago, the crew of Medic 92, crouch down beside her. “What’s the matter?” Samuel asks.
She clenches a hand low on her abdomen. “I got a pain. Down here. So bad I can hardly….” She breaks off, wheezing.
“How long has that been going on?”
“A couple of days. I—it just got so bad….”
“OK,” Samuel says. “Let’s see if we can get you outside.”
Samuel puts a gloved hand under her elbow. With Manago at her other side, she gets shakily to her feet. Every step makes her wince and pant, and it’s a slow walk out to the ambulance. Her face is tight with pain; only once she is settled on her back in the stretcher does she open her eyes again.
Samuel palpates her belly gently with his gloved palm. “Does this hurt? And here?”
It seems to hurt everywhere. He asks if she has ever had a urinary tract infection.
No, she says, but she has had kidney stones for seven years. “I pass one at least once a year,” she says. “Not less. More, sometimes.”
“Have you noticed any blood in your urine?”
“A tinge. It was pink, pinkish.”
“How long?”
“Ten days.”
Manago puts a hand under her shoulder to help her sit up, and she screams. “Don’t touch there,” she says. “I got a really bad bruise. I got bruises on my shoulder and one on my knee, and on my buttocks, where my ex-boyfriend hit me with a steel pipe.” She pulls up the leg of her shorts and turns over to expose an ugly, precise purple stripe at the top of her thigh.
She has no insurance, no address except her mother’s house in Louisiana, and no regular physician, though she has had plenty of doctors: for viral meningitis, for Hepatitis A, for an E. coli infection in her kidneys, three Caesarean sections, a hysterectomy, an appendectomy, and gall bladder surgery.
Samuel asks her to make a fist as Manago uncoils the long, clear tubing on a saline drip.
“You’re not going to find a vein,” she warns them. “Nobody can find one. I had a nurse try to find one, she put a needle all the way through my vein into my arm.”
“Let us try,” Samuel says. He tourniquets her arms with a strip of latex and holds her hand, watching for an artery to pop up. It doesn’t. He puts her arm down.
“Are you allergic to any medications?”
“Eight,” she says, and rattles off the list, which includes a few sedatives and most major painkillers.
“Anything else wrong?”
Yes. She also had a headache.

They take her to one of the smaller regional emergency rooms. The nurse administrator frowns at them as they wheel their patient in—it’s their second drop-off to this ER in the last few hours, and the hospital is trying to divert. Diversion is a courtesy extended by ambulance crews; while they try to honor hospitals’ requests to take patients somewhere else, sometimes there’s little choice. If a patient is in critical condition or severe pain, the ambulance goes to the closest hospital. If a patient has a complicated history, and their paperwork is at one hospital, EMS will take the patient there, to avoid expensive and time-consuming duplication of tests. And if patients request a specific hospital, the ambulance crew must take them there, by law.
A good hour before sunset, the ER is already over-flowing. Patients are parked on gurneys in the hall—two skinny, corn-rowed teenagers and their fussy baby, an old woman whose husband stands by her, rubbing her feet, a woman with a small, coughing girl on her lap. Small emergency centers like this one are some of the hardest hit by systemic overcrowding, a 2002 study by Save Our ERs found. These smaller emergency facilities typically don’t have the equipment or staff to handle the most severe trauma cases, and must transfer those severely injured patients to bigger ERs, like the one at Ben Taub. Transfer is a lengthy and paperwork-heavy process at the best of times. When the receiving ERs are crowded themselves, a transfer can add as much as five hours to the patient’s wait for care. Save Our ERs found nearly all small ERs in Harris County routinely had trouble transferring patients to larger emergency departments. Two out of three small ERs reported that delays endangered patients’ health. Delays also meant patients might need more intensive—and costly—stabilization treatment after the transfer.
This evening Samuel and Manago wait 35 minutes to sign their patient over to the ER nurses. ER staff are not supposed to keep ambulances waiting more than 30 minutes—a practice EMS workers call “parking ambulances”—but it’s not unknown for ambulances to be parked an hour or more when ERs are slammed. Meanwhile, from the safety of the gurney, the woman with the abdominal pain relaxes, becoming talkative, even a bit flirtatious. Finally, Samuel and Manago get a green light to roll their charge down the hall and into an observation room. With two nurses’ help, they shift the wincing woman into a bed. “Good luck,” they tell her, and head back down the hall. She waves goodbye.
A nurse, with her hands on her hips, calls after them, “Don’t come back.” She laughs, and so do they, but she seems to be only half joking.
Back at the station, the hardest part is waiting. There’s no knowing when a call will come in, but it’s Sunday night—the last good party night of the long holiday weekend—and the crew is braced for a busy shift. Their pagers flash on and off, alerting them that yet another hospital is on diversion. There are a couple of false alarms—a drunk driver who hit a parked car but is unhurt, a man whose neck was clawed in a domestic dispute in a housing project. Both men turn down a trip to the hospital.
A little before midnight, a call comes in for a diabetic in hypoglycemic shock. When Samuel and Manago arrive at the house, they find a woman in a pastel plaid nightgown sprawled on a queen-sized mattress just inside the front door. A wall-sized television gives the room it’s only ghostly light. The woman’s husband sits next to her, trying to feed her a peppermint. Three adult daughters hover nearby. Here and there around the room are boxes of snack cakes. A half-finished loaf of white bread in its plastic wrapper sits on the back of the sofa.
“How long has she been unconscious?” Manago asks.
A few minutes, the family says. They explain that she often wakes up woozy from low blood sugar. Usually she manages to eat something to keep her from fainting.
“Has she eaten today?” Samuel asks.
One daughter says yes, and another, no. The husband is consulted; he thinks not. “She wasn’t hungry,” he says.
Manago squeezes a tube of medicinal glucose—sugar gel—into the woman’s slack mouth, while Samuel pricks her finger to take a blood sugar test. She’ll be conscious in a minute, they reassure the family. There’s no need to take her to the hospital tonight. But she should have something to eat.
“Do you have anything like orange juice?” Samuel asks.
The oldest daughter shakes her head.
Samuel tries to do some quick patient education. “You have simple sugars and complex sugars,” he instructs. “The simple sugars, she’s going to burn through them very fast. You need to make sure she also gets complex sugars. Not peppermint.”
Patients who receive their primary care from ambulances and emergency rooms receive their health education from doctors and nurses in a hurry, mostly concerned with stabilizing the immediate crisis. They rarely have time to provide patients with comprehensive information about how to manage chronic illnesses, or prevent the acute episodes that bring them to the emergency room over and over again.
The oldest daughter unpockets a roll of bills. “Here,” she tells her sister. “Go get some juice. They say she needs orange juice.”
It’s Tuesday morning. Labor Day weekend is over but the rush on Ben Taub’s emergency center hasn’t slowed down—in fact, it seems to be picking up. The hospital’s newly expanded waiting area is almost standing room only. “People wonder why we don’t just build more, add more beds, but it’s like squeezing a marshmallow,” George Masi says. “If you build more clinics, that will generate more referrals to the emergency centers, and vice versa. If you increase capacity anywhere, you have to increase capacity everywhere.”
In the next decade or so, the hospital district hopes to triple in size, adding two more trauma centers and 11 community clinics. But there’s also the delicate matter of finances. As hospitals take on more and more patients for whom no one can or will pay—neither the state, the insurance companies, nor the sick people themselves—their budgets are tipping precariously into the red. Masi estimates that as much as 60 percent of the care Ben Taub provides is never paid for, with that percentage perhaps slightly higher in the emergency center. On average, the hospital loses money for every patient treated in the emergency center. The more the hospital expands emergency services, the more they stand to lose. “It is a challenge for us,” Masi says. “How do we continue to grow, do more, and not go into bankruptcy? It’s a delicate balance.”
Texas trauma centers provided $180 million in uncompensated care in 2001, according to a study commissioned by Save Our ERs from healthcare consultants Bishop + Associates. Most of the uncompensated care is provided to the medically indigent—those without state aid or third-party insurance, who can’t afford to pay for their care themselves. However, a good portion of Texas hospitals’ debt is generated by insurance companies and by the state itself. Health Management Organizations employ strategies—known as gate-keeping—to dodge payments to hospitals. Originally intended simply to control costs, gate-keeping practices are now notorious for delaying or avoiding legitimate payments to hospitals and physicians. HMOs may require hospitals to obtain prior consent from the liable insurance company before providing a patient with a treatment or service. While the hospital waits for authorization, the untreated patient’s condition may worsen, necessitating yet more expensive stabilization and treatment. If the hospital treats the patient without authorization, the HMO may decline to pay. HMOs are also known to refuse payment for emergency services provided for illnesses that prove not to be life threatening. If the classic symptoms of a heart-attack—chest pains, nausea, shortness of breath—turn out to be an attack of indigestion, the HMO may not pay for treatment received at an emergency center, since the condition treated was never an “emergency.” Some insurance companies accept charges only to delay payment to physicians for months or even years at a time.
The state itself has lately been a poor patron to Texas hospitals. Texas used to draw down federal matching dollars to provide funds to hospitals that served higher than average numbers of uninsured and medically needy patients, but over the last decade that funding has declined steadily. The amount the state reimburses hospitals for treating Medicaid patients has also shrunk. In 2002, low Medicaid reimbursement rates resulted in a $27.2-million loss for Texas trauma centers, one study from Save Our ERs shows. Add to that the last legislative session’s cuts to Medicaid, CHIP, mental health, and geriatric services. (State reductions in CHIP collections alone have meant a $36-million loss to the Harris County Hospital District in the current budget cycle.) Inevitably, each cut in state spending on healthcare generates trips to the ER by sick people who now have nowhere else to go.
“Every reduction in reimbursement is a very painful outcome for us,” Masi says.
In 2002, Texas hospitals spent $6.5 billion on uncompensated care. While tax-supported hospitals may be able to raise taxes to generate revenue, private hospitals or those with smaller tax-bases may simply be forced to close. Since 2000, 13 Texas general hospitals have closed. Eight more have downgraded their emergency departments to lower levels that allow them to offer less intensive care, or closed their ERs altogether.
The huge load of debt hospitals swallow only increases the crowding in emergency centers. Most hospitals try to recoup some of their losses by charging more from those who can pay—the insurance companies of insured patients. In turn, insurance companies keep margins up by increasing the cost of health insurance premiums. The high cost of premiums causes many small businesses to drop policies on their employees. The newly uninsured struggle along until they get sick—then they go to the emergency room.
Houston’s chamber of commerce, the Greater Houston Partnership, has called for several fixes to Harris County’s floundering healthcare system, including integrating hospitals’ record-keeping systems and expanding hours at community clinics. By far the most ambitious part of the plan, however, is to extend insurance to more of the population. It’s a good idea, obviously. But without considerable state and federal effort, it’s hard to see how it will happen. So far, nothing approaching universal healthcare is on the state’s agenda for the upcoming 79th legislative session. Indeed, the Texas Department of Health Services’ funding requests for CHIP and Medicaid in 2006 and 2007 would barely cover the costs of inflation.
The state’s emergency rooms are the last landing places in a safety-net system whose holes are getting bigger all the time. They will not hold much more strain. “I expect this to get steadily worse,” says Dr. Clifton of Save Our ERs. “It will become intolerable. Everyone will be affected.” Clifton believes lives are already lost in emergency rooms because physicians and nurses cannot treat patients in time. He foresees an emergency system in which patients wait for hours in ambulances at hospital loading docks, where patients are past saving before they reach the observation bed. And anyone—rich or poor—who ends up in an emergency room will suffer. “On a good day you’ll get prompt care, and on a bad day you won’t. You won’t know what kind of day it is until something happens to you. All you’ll know is that everyone did everything they could, and it still took four hours to see Grandpa, and now he’s dead,” Clifton says.
At the new triage station in Ben Taub’s new waiting room this Tuesday morning after Labor Day, nurses work with the controlled hysteria of people inured to permanent crisis. On the other side of the counter, a wall of hurt people plead illnesses comprehensible and incomprehensible, deadly, trivial, or partly imagined: Grippe. Mala sangre. “My stomach is sour.” “I hurt so bad I can’t stand up.” Fever. Stabbing pains. “I’m out of my medication and now I have an infection.” “There’s a balloon in my bladder.”
A woman who has been hovering around the desk for several minutes stretches her arms across the counter, thrusting clasped hands into one nurse’s face. “Listen,” she says. “My husband’s having a heart attack. He can’t breathe. He’s throwing up.”
The nurse freezes, her hand in midair above a stack of papers. “He has heart failure?”
“Yes.” The woman turns around and beckons to her husband, who is sitting down. He stands up wearily and comes forward. He is a massive man, both tall and wide. She puts her arms around him as far as they will go. Sweat stains stretch from under his arms all the way across his chest. Beads of sweat roll down his temples.
“Have you been diagnosed with heart disease?” the nurse wants to know.
He nods.
“Are you having trouble breathing?”
“Yes.”
“Do you have pain right now?”
“Yes.”
“Where?”
He puts his hand over his sternum, makes a circle from his throat to the middle of his chest. “All over here,” he says.
“What’s your number?”
“Forty-six.”
She looks down at her clipboard, at all the names ahead of his, blinks, and makes a decision. She pulls up a blank patient information screen on the computer. “What’s your name?” she asks. Five minutes later, an aide comes out and leads the man into the back. He may not see the doctor right away, but he is through the first hurdle.
Those not fortunate enough to be having a heart attack still wait, hunched in their seats or pacing in the halls. The wait will be many, many hours. But they will wait, because, while they are not all equally sick, they are all afraid. Everyone, in fact, is here because of an emergency—the emergency of a broken leg, or the emergency of having nowhere else to go.
Emily Pyle is a writer based in Austin.
LIFELINES
On Saturday afternoon, six nurses in scrubs man five telephones in an office carousel on the third floor at Ben Taub. The extra nurse, Victoria Chavis, is training a recent hire how to perform emergency room triage over the telephone. As patients call the hotline from home, nurses enter their names and personal information into a computer database. A series of computer menus guide nurses through the triage questioning process—What are your symptoms? How long has that been going on? How much does it hurt? What medications are you taking? Depending on the answers, nurses may advise patients to care for themselves at home, or see a doctor within a few days; if the case is urgent, they may recommend the patient go to the emergency room, or even call 911. But the main purpose of the Ask Your Nurse Hotline—started three years ago by Gateway to Care, now staffed and operated by the LBJ Hospital—is to keep non-emergencies out of the emergency room.

As Chavis listens in on an operator’s headset, trainee Sharon Powe fields a call from a woman with pain and swelling in her shoulder. The woman has a history of seizures; it’s possible she fell during one and injured herself, but she doesn’t remember the fall. “Is it red?” Powe asks. “Is there swelling?” The woman says yes to both.
“Are you taking any medications for it?” Powe asks.
“Percoset,” the patient says. “I took two tabs. I’m just falling out right now.”
With Chavis’ occasional sotto voce guidance, Powe steers the woman through the rest of the litany of questioning, then recommends that she see a doctor within a few hours. Since this is the weekend, that means the ER. The woman tells Powe that she called the ambulance that morning, after she had a spell of dizziness. They didn’t take her to the hospital, she says, insisting instead that the dizziness was just high blood pressure brought on by anxiety.
“Sorry to hear that,” Powe says. “Sorry that happened.”
After some extra soothing, the woman ends the call. Chavis, a small woman with perfectly round glasses and a Cheshire grin, turns in her chair. “That was one of those complicated cases we get a lot of. They give you their symptoms all jumbled up. ‘I have this, and I have this…’ You have to ask a lot of questions to sort it out.”
Powe, who has 23 years experience in conventional ER triage, nods agreement. “You have to make the patient be your eyes and ears,” she says. Nurses working the hotline have asked callers to cough into the phone, or to hold the receiver against their babies’ chests, so nurses can hear them wheezing.
The hotline (713-633-CALL) started three years ago. In August 2003, it began to offer its service 24 hours a day. About 2,500 calls were answered this June, up from 1,500 just six months earlier. About a third of those calls are “information only”—callers with general questions about an illness or medication. Of the remainder, around 40 percent are referred to the emergency room or told to call 911. This year to date, the hotline has prevented about 3,000 unnecessary trips to area emergency rooms. Hotline nurses also provide a service unheard of at emergency rooms and even most clinics: A day or so later, they call patients back to make sure they’re okay.
Powe takes a quick break and Chavis answers a call from a woman whose son has been stung by a bee at a picnic. The boy is breathing normally and swelling is contained to the site of the sting, so Chavis recommends removing the stinger with a credit card and applying a paste of baking soda and water to the sting. Benadryl, she says, will take care of swelling. No need to go to the hospital unless something gets worse. The caller hangs up, reassured.
“That call probably would have been an ER visit,” Chavis says. “She was scared and she didn’t have anyone else to call.”


