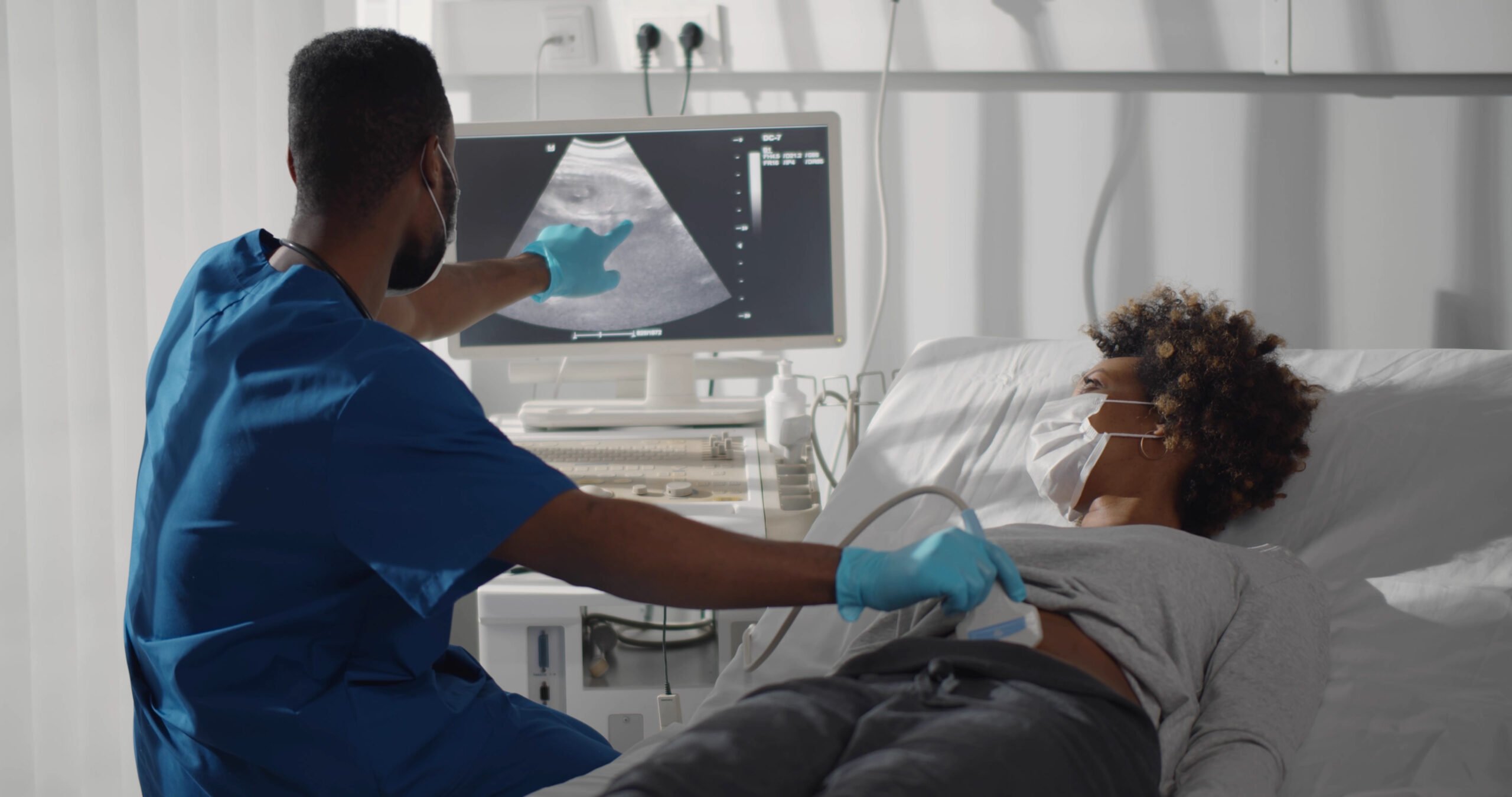
Report: If Rural Texans Want Decent Health Care, They Should Mosey to New Hampshire
With high rates of fatal heart disease and stroke, limited access to care and sky-high uninsured rates, Texas gets a “D-” in a new “report card” comparing rural health care between states.

Texas and other Southern states are home to small-town doctor shortages, skyrocketing rates of preventable disease among rural residents and some of the highest uninsured rates in the nation, according to a new report that places Texas’ rural health care failings in a national context for the first time.
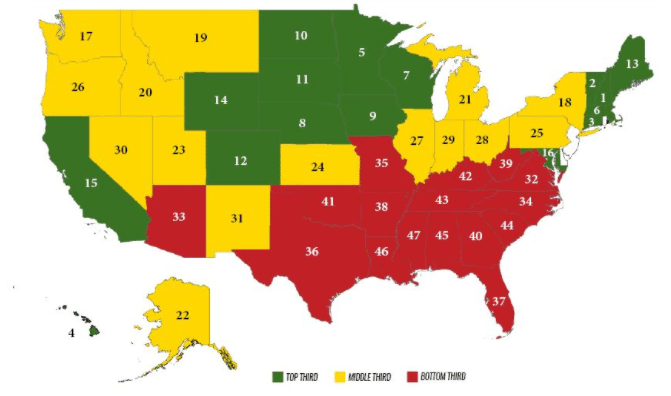
The “report card,” published last month by researchers at Texas Tech University’s F. Marie Hall Institute for Rural and Community Health, examines each state’s rural health care in terms of mortality, quality of life and access to care. Texas was slapped with a grade of “D-” and ranked 36th out of 47 states (New Jersey, Delaware and Rhode Island were not included in the analysis for lack of rural counties). Among other factors, Texas was dinged for high rates of death from heart disease and stroke in rural areas.
New Hampshire, with plentiful access to rural doctors and a relatively low uninsured rate, was ranked No. 1, followed by Vermont and Connecticut, respectively.
Advocates have for years called on the Texas Legislature to address crumbling rural health care in the state, where in some cases residents must drive hours to the nearest hospital. Despite advocates’ efforts, small towns have been plagued by a wave of hospital closures, at least 18 since 2013. That problem likely will be exacerbated when funding — provided by a critical Medicaid waiver program — to the remaining facilities is cut in the near future.
“I wish I could say that we were surprised, but it was sort of the suspicion that Texas has been struggling with rural health care for years,” said Texas Tech researcher Scott Phillips. “We wanted to know how well Texas stacked up against the rest of the nation, and that data just wasn’t available. … No one had tried to do a comparative analysis across the nation before.”
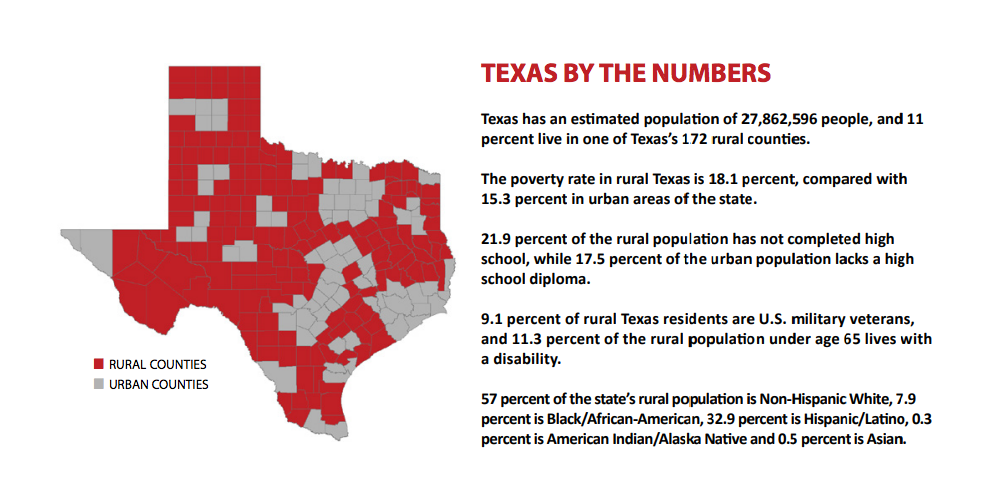
The analysis included such factors as leading causes of death (in Texas, it’s heart disease), residents’ self-reported health problems, the number of doctors in rural counties and the state’s uninsured rate. Texas earned an “F” in the “access to care” category, including access to rural physicians, mental health professionals and dentists. Eighty Texas counties have five or fewer doctors, and 35 have no doctor at all, the most recent figures show.
Researchers found that Texas’ rural uninsured rate for people under 65 is the second-worst in the United States — 25.3 percent of rural Texans under age 65 are uninsured, compared to an urban rate of 22.6 percent, which is the worst in the country. Nationally, the uninsured rate — in both urban and rural communities — is about 12 percent, according to a Gallup poll published Tuesday.
The report also found wide disparities between Texas and other states regarding rural mortality rates for heart disease and stroke, two leading causes of death that “are among the most preventable,” according to the U.S. Office of Disease Prevention and Health Promotion. Rural Texans die from heart disease at a rate of 210 deaths per 100,000 people, well above the national rural rate of 169 deaths. The state’s stroke mortality rate is also above average: 47 deaths per 100,000 compared to 38.
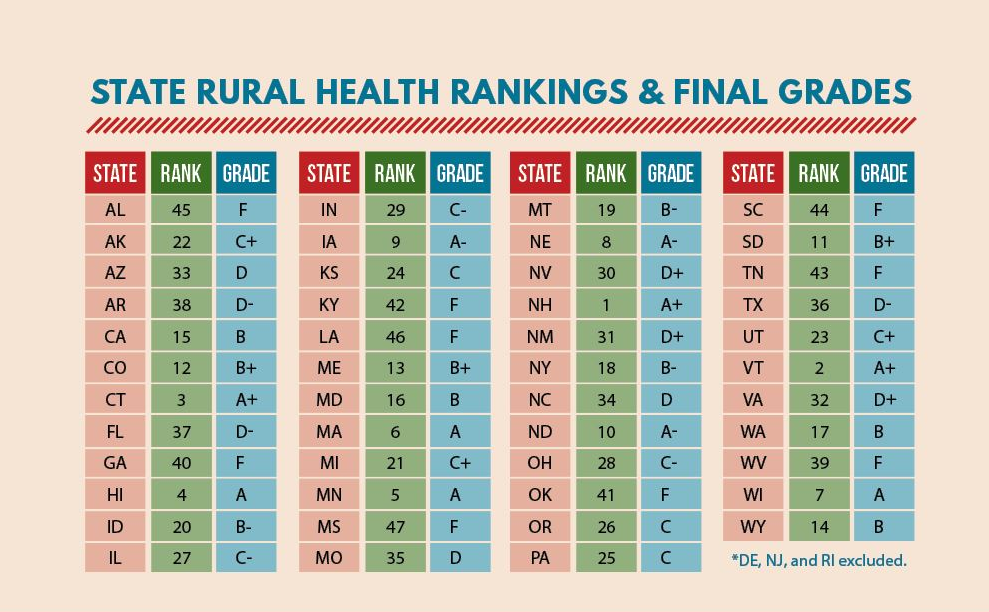
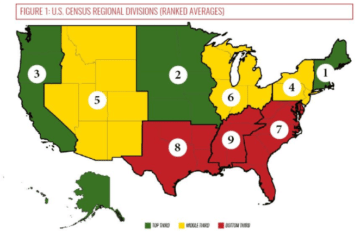
Phillips’ said one of the study’s most interesting — and befuddling — findings is that in almost every instance, states in close geographic proximity earned similar grades. The worst-performing states (with the exception of Arizona) were in the South, with low performers including Lousiana, Mississippi, Georgia, Oklahoma and South Carolina. Northeastern states earned stellar grades, as did Minnesota and states surrounding it in the Upper Midwest.
“Everything clustered together into these regional groups. It seems like the greatest prediction of your state’s grade is the grade of the state next to you,” Phillips said. A state’s region appeared to be an even better indicator for rural health care success than whether a state opted to expand Medicaid under the Affordable Care Act. Texas declined to expand Medicaid under the law, but its neighbor, Louisiana, received the second-lowest ranking in the study, despite expanding Medicaid.
Phillips said more research is needed to explain the trend, but he hopes that the study’s findings will serve as a springboard for improvements to rural health care nationwide.
“We thought it was important to lay all that data out there for decision-makers to see,” Phillips said. “One of our primary goals is to effect change… The more we prioritize getting care into rural communities, the more lives we can affect.”