Rural health care is in crisis around the country, but Texas is suffering the most. At least 20 small-town hospitals have closed since 2013. More than one-fifth of Texas’ 254 counties have only one doctor or none at all. State lawmakers have the tools to slow or reverse the trend, but they’ve mostly neglected to use them. The result? Without nearby medical services, many of Texas’ rural residents end up traveling hours for care—and because of this, people are dying.
Towns are too. Rural communities need health care in order to attract businesses and create jobs. But newly graduated doctors are often averse to working in tiny, down-on-their-luck communities. No doctors means no hospitals, and no hospitals means few businesses. The vicious cycle goes on.
Much has been written about medical deserts, but we’ve rarely heard from the people who call them home. This series highlights the stories of rural Texans without access to care—and explores what can be done to reverse this troubling trend. The Texas Observer will continue reporting on rural health care in the coming months.
Part 1
A Dying Town

When a hospital shuts down, everyone in the community loses—the insured and uninsured alike. The hospitals in Clarksville, Gilmer, and Mount Vernon, which closed simultaneously in December 2014, are now in various stages of disrepair. The Clarksville building is a mere skeleton; the steel support beams and concrete floors are all that remains of the three-story structure. It’s an apt symbol for the town of Clarksville, where factories and manufacturers have packed up and moved to other towns with better highway access. Even the Walmart on Highway 82 is vacant. Local public officials say it’s difficult to recruit businesses to set up shop in a town with no functional hospital. In Gilmer, an hour southeast of Clarksville, what was once a hospital is now an empty lot; the building has been ripped out, foundation and all. Read more.
Scenes From A Rural Hospital’s Final Day
It’s July 22, and Chillicothe Hospital is closing. Built around 70 years ago, the hospital has been forced to accept fewer and fewer patients because there aren’t enough nurses to see them. This trend is mirrored in the surrounding town of Chillicothe, which has hemorrhaged half its population in recent years. With so few patients to bring in revenue, the hospital can’t make ends meet. Recently, visitors who do come have been met with a paper sign taped to the front door, directing them to the closest hospitals about 20 minutes away. Read more.
Part 2
Driving My Life Away

Texas is facing a critical physician shortage. Two decades ago, 14 of the state’s 254 counties had no doctor. Today, that number has jumped to 33. More than 20 other counties have just one. In 2018, Texas had about 54 primary care physicians per 100,000 people, according to research from the Robert Graham Center, affiliated with the American Academy of Family Physicians—one of the lowest ratios in the country and far below the national ratio of 76 per 100,000. For years, medical professionals have been sounding the alarm, but they say lawmakers are still not doing enough to bring services to far-flung Texas—and that the problem is only getting worse. Read more.
The Rural Health Care Crisis, Mapped
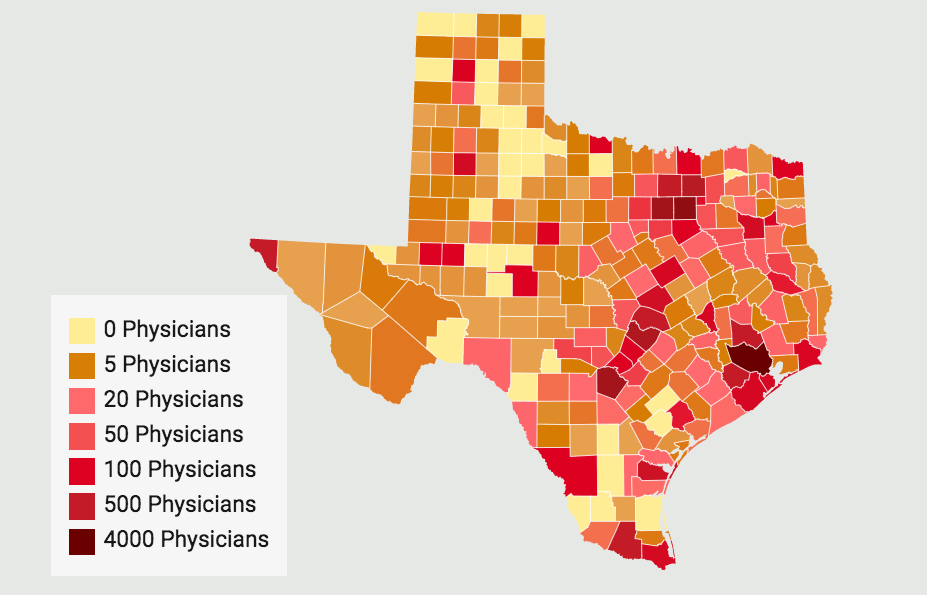
Rural Americans bear the brunt of the country’s doctor shortage—and in Texas, home to the largest rural population of any state, it’s especially acute. More than one-fifth of Texas’ 254 counties have only one doctor or none at all. Using data from the Texas Department of Health Services, we mapped the number of primary care physicians per county in Texas. The county colors range from yellow—zero physicians—to maroon and dark red, where there is a heavy concentration of doctors. These “hot spots” are in urban areas of the state, such as Harris, Bexar, and Dallas County. Read more.
The Last Nurse in Memphis, Texas

Carole Ward, a 66-year-old nurse practitioner who lives in Hedley, ran the Memphis health clinic from 2005 until she retired and the clinic closed in 2017. The clinic offered limited services, but it was better than nothing. In the two years since, Hall County officials have been trying to reopen it, with some advocates suggesting loosening restrictions placed on mid-level practitioners such as Ward. Under Texas law, nurse practitioners and physician assistants can render medical services under the supervision of a licensed physician. In late July, the Observer sat down with Ward to talk rural health care, running a small health clinic, and her decision to leave the facility. Read more.
Part 3
Labor Away
Like many other parts of rural Texas, Ozona is caught in the middle of a devastating health care crisis. The town lost its hospital in 1996, leaving it to rely on a single health clinic that offers limited reproductive health services. People seeking basic preventative services or prenatal check-ups typically need to make a 170-mile round trip drive to San Angelo, a mid-sized city to the northeast. Pregnant patients have to make the same hour-long drive to give birth. The closest abortion clinic is in San Antonio, a 400-mile round trip. The reproductive health care problem in Ozona is notably pernicious, but millions of rural Texans lack access to these services. More than half of Texas counties have no OB-GYN. Of the state’s 158 remaining rural hospitals, just 66 still deliver babies, according to the Texas Organization of Rural and Community Hospitals. Read more.
We Asked You About Health Care in Rural Texas. Here are Your Stories.

Reporters Sophie Novack and Christopher Collins spent months digging into Texas’ rural health care crisis. Throughout their reporting process, we asked readers to share their experiences seeking care in far-flung parts of the states. We heard stories about doctor shortages, hospital closures, and insurance troubles. Many rural Texans told us they struggled to find coverage near their homes and were forced to make hours-long drives to reach necessary providers. These are some of their stories. Read more.



